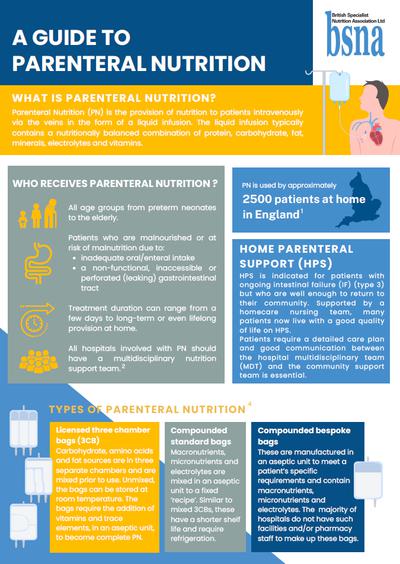
Parenteral Nutrition (PN) is often referred to as Total Parental Nutrition (TPN) which implies that this is the sole source of nutrition; in some cases, patients on PN may receive a small amount of nutrition via the gastrointestinal tract.
"A multi-disciplinary team of clinicians, dietitians, nutrition nurse specialists and pharmacists are required to establish, monitor and manage patients on parenteral nutrition in the acute setting."
Parenteral nutrition is used when patients have an inaccessible or non-functioning gastrointestinal system.
The National Institute for Clinical Excellence (NICE) recommends that healthcare professionals should consider parenteral nutrition for patients who are malnourished or at risk of malnutrition and have an inadequate or unsafe oral and/or enteral nutritional intake, or a non-functional, inaccessible or perforated (leaking) gastrointestinal tract.
Parenteral nutrition is delivered to the patient’s bloodstream through an intravenous catheter, which is ideally placed centrally into a large vein near the heart; this is usually called a central line or a peripherally inserted central catheter (PICC). Less frequently, smaller veins further from the heart are used; this is called peripheral administration. Safe intravenous access and catheter care is essential to minimise the risk of complications and infection.
Some patients may require parenteral nutrition on a long term basis and may be discharged on home parenteral nutrition. For those patients whose gastrointestinal function improves or recovers, parenteral nutrition may be gradually withdrawn, but only once adequate oral or enteral nutrition is tolerated and nutritional status is stable.
Nutritional Regimens

Standardised ranges of compounded parenteral nutrition regimens are available for both adults and newborn children and are tolerated by a broad spectrum of patients. Parenteral nutrition may also be specifically tailored to a patient’s nutritional needs; an accurate assessment of a patient’s nutritional needs is required to ascertain the precise composition of the nutrition. For this reason, regular monitoring of the patient’s biochemistry and fluid balance is essential.
The stability of the PN bags is affected by volume and the proportion of the constituents, especially amino acids and fat, amino acid formulation, glucose and electrolytes.
Parenteral nutrition is governed by pharmaceutical law. The Medicines and Healthcare Regulatory Authority (MHRA) is the UK body responsible for authorisation and regulation of products and associated devices.
A list of the courses available for healthcare professionals in the UK can be viewed here: Parenteral Nutrition Training Dates 2026.
Transitioning from Hospital to Home on Parenteral Nutrition
The British Specialist Nutrition Association (BSNA)* has developed two educational video animations to explain how patients receiving parenteral support in hospital can effectively manage their treatment at home once discharged from hospital, including what to expect at every stage of their journey. The video is a guide for patients and caregivers and can be used to help answer any questions the patient or caregiver may have.
*BSNA Member Companies involved in the creation and funding of the videos are B Braun, Baxter and Fresenius Kabi, with input and review from PINNT
1. Home Parenteral Support (HPS) for shorter term use - A transition from hospital to home
This educational video provides patients and caregivers with information on what to expect when transitioning from hospital to home on parenteral support where parenteral support may be stopped for a number of reasons, which will be discussed and agreed with their Nurses and their Nutrition Support Team.
2. Home Parenteral Support (HPS) for long term use - A transition from hospital to home
This educational video provides patients and caregivers with information on what to expect when transitioning from hospital to home on parenteral support where parenteral support is expected to be used long term.
ESPGHAN Parenteral Nutrition Series

Home Parenteral Nutrition

Organisational Aspects of Parenteral Nutrition
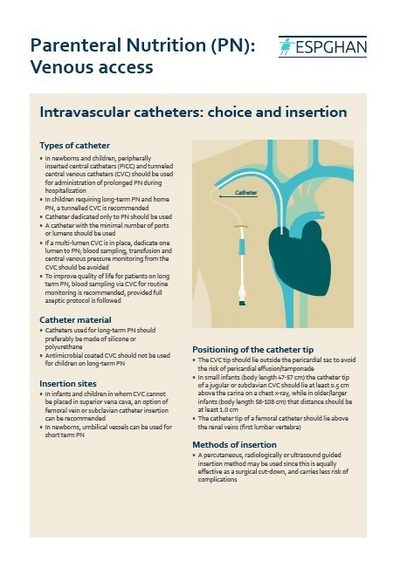
Parenteral Nutrition - Venous Access

Complications of Parenteral Nutrition
Webinars
You can access BSNA's previous webinars below:
Webinar Part 1 - Parenteral nutrition use in advanced cancer
Parenteral Nutrition in Advanced Cancer: Decision Making: Should PN be started?
This webinar explores the rational and background of starting patients with advance malignancy on nutritional support. It evaluates the different forms of nutritional support with the focus on parenteral nutrition. It demonstrates and interrogates the existing guidelines available and relate this to the practice, along with providing key messages for managing patients with advance malignancies.
Webinar Part 2 - Parenteral nutrition use in advanced cancer
Parenteral Nutrition in Advanced Cancer: How to facilitate PN in advanced Cancer
This webinar explores the practicalities of establishing patients with advanced malignancies on parenteral nutritional support, demonstrating how team work can facilitate a smooth and uncomplicated discharge pathway, with particular focus on the very difficult decision making of stopping parenteral nutrition support towards the end of life.